Introduction
Kawasaki disease (KD) is a systemic vasculitis and is currently a leading cause of acquired heart disease in children. Its etiology is presumed to be related to the infection of a genetically susceptible host. However, a diagnosis of KD is made based on clinical manifestations, and it is mandatory to rule out underlying diseases. It is sometimes very difficult to make a differential diagnosis of the clinical signs and remains challenge to determine whether such clinical signs arise from KD or viral or bacterial infections. Clinical manifestations vary depending on the age of the affected patient. Therefore, it is important to carefully monitor clinical clues of KD, especially in very young patients (e.g., infants less than 3 months of age) and older children outside the dominant age range for KD [1]. Furthermore, when the patient shows recurrent episodes of KD, further evaluation is essential to rule out recurrent infection or rheumatologic disease showing a similar clinical course.
We report a case of a 6-year-old boy who initially presented with a painful erythematous neck mass that progressed to be diagnosed with KD, repeated three times, along with retropharyngeal edema on computed tomography (CT) and pathologic findings of lymph node (LN) biopsy.
Case
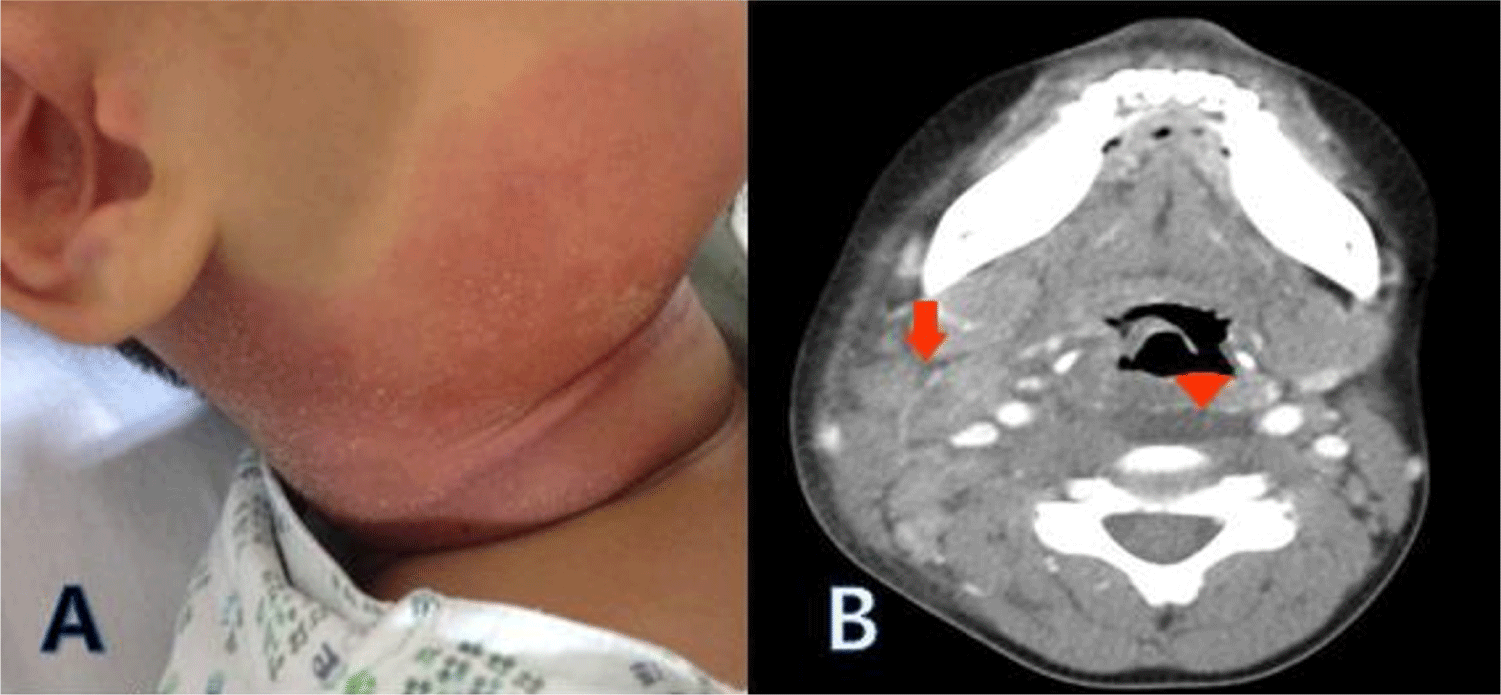
A 6-year-old boy presented with a painful neck mass accompanied by fever, dysphagia, and limited neck motion for 2 days. The patient had been well until this admission. He had already experienced two episodes of unilateral huge neck mass for which he underwent computed tomography (CT) scan two years ago, one of which was diagnosed with KD. The patient displayed a heart rate of 100 beats per minute, a body temperature of 37.9℃, and a blood pressure of 90/50 mmHg. Other than a tender mass on the right neck, the patient showed non-specific symptoms. The patient was treated with antibiotics including clindamycin and a third generation of cephalosporin. However, the patient continued to have a fever and developed a markedly enlarging tender cervical mass with severe skin erythema, as shown in Fig. 1A. With limited neck motion and dysphagia, the patient underwent a CT scan of the neck which revealed a deep neck infection in the retropharyngeal space and submandibular space, with enlargement of multiple lymph nodes (Fig. 1B). Laboratory findings showed a white blood cell count of 17,830 /mm3, with 82.3% segmented neutrophils, hemoglobin level of 11.4 g/dL, and platelet count of 323,000 /mm3. C-reactive protein level was 23.4 mg/dL (with a normal range of 0−0.3 mg/dL), and the erythrocyte sedimentation rate was 86 mm/h. While the serum level of amylase was mildly elevated at 167 U/L, the levels of aspartate aminotransferase, alanine aminotransferase, and other biochemical markers were within normal limits. Despite the administration of antibiotics, the patient’s body temperature reached 40℃, the redness of the skin around the neck mass worsened, and retropharyngeal edema was confirmed on CT. Amikacin was added two days later, but the fever and redness continued to worsen. Blood tests were performed every 2−3 days, and on the 6th day after the onset of fever, the CRP level peaked at 23.5 mg/dL. The patient had a history of two episodes of recurrent cervical lymphadenitis which had been diagnosed with KD without coronary arterial complication, and the current neck mass progressed to a deep neck infection, for which he underwent a lymph node biopsy. During the operation, the patient had a serous discharge from the edematous phlegmon in the retropharyngeal space. The patient finally presented a conjunctival injection and mild redness of the lips on the 6th day of fever. On the 7th day of fever, the patient displayed typical KD findings, such as redness of the eyes, lips, and tongue, as well as redness of the hands and feet, fulfilling diagnostic criteria for KD. An echocardiogram showed increased perivascular echogenicity around the right and left coronary arteries, along with trivial mitral valve insufficiency and a small amount of pericardial effusion. Despite receiving antibiotics, the patient’s clinical condition deteriorate, and the lesion pattern observed during the cervical lymph node biopsy was not purulent. Therefore, based on the results of the echocardiogram and clinical symptoms that met the typical diagnostic criteria for KD, the administration of antibiotics were discontinued, and the patient was given intravenous immune globulins (2 grams/kg) along with a high dose of aspirin. The following day, the patient’s fever subsided completely without the need for antibiotics.
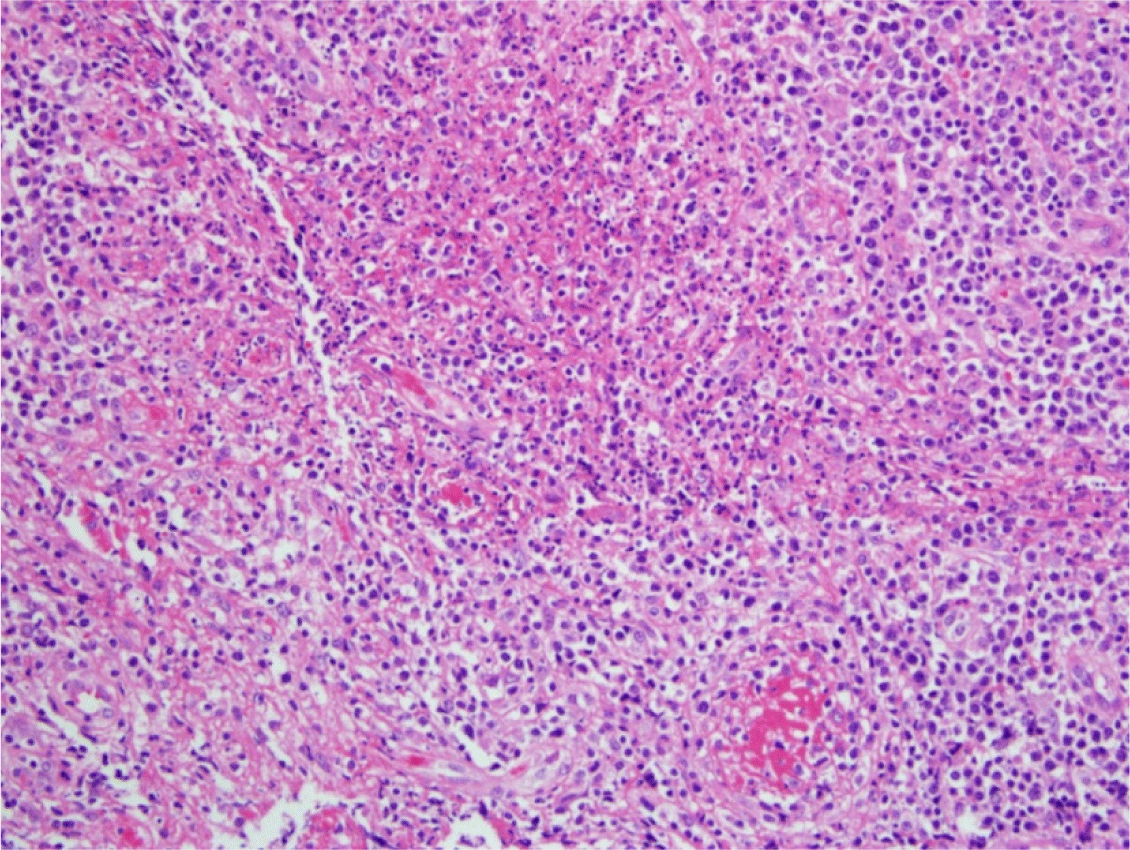
The histopathologic findings of the lymph nodes were suggestive of focal necrosis with fibrin thrombi in small blood vessels accompanied by nuclear debris, indicative of lymphadenitis with vasculitis on Hematoxylin and Eosin (H&E) staining (Fig. 2). The in situ hybridization study of Epstein-Barr virus for lymph nodes was negative. Blood cultures and PCR tests for nine types of respiratory viruses, as well as serologic tests for EBV, HIV, mumps virus, and anti-nuclear antibodies, showed negative results. With a gradual decrease in acute reactants, platelet counts increased gradually, followed by typical desquamation of the fingertips. The patient exhibited no coronary arterial complications and showed complete remission of the valvular regurgitation and pericardial effusion in the follow-up echocardiography. The patient showed typical features of KD, including abnormal echocardiogram findings, increased platelet counts, and finally showed typical thick subungual desquamation.
Discussion
In cases of progressive suppurative cervical lymphadenitis despite antibiotics treatment, where no pathogens are detected, it can be challenging to choose proper antibiotics for the next step. The patient reported herein had two episodes of cervical lymphadenopathy which had progressed to KD, but had no clinical features of KD until a lymph node biopsy was performed. Finally, the symptoms resolved with IVIG infusion without antibiotics. While it is not difficult to diagnose KD in the age groups where it often occurs, diagnosing KD in age group outside the prevalent range of the disease can be challenging, particularly in patients with only partial clinical symptoms [1]. According to Fan et al., school-aged children are susceptible to developing cervical mass as one of the initial presentations of KD, which indicates an increased risk of developing coronary arterial complications [2]. In clinical settings, we occasionally encounter patients with suppurative cervical lymphadenitis that progressively manifest clinical features of KD, often referred ‘node-first KD’ [3]. Our case is noteworthy for the following reasons: the patient presented with a deep neck infection on the imaging studies, a tender mass, and limited motion in the right neck concurrently. Despite receiving additional antibiotics other than clindamycin and the third generation of cephalosporin, the patient’s clinical course did not improve. Evidence that the patient’s cervical lesion was not a suppurative bacterial infection was suggested by a serous aspiration specimen of the cervical lesion, CT findings of retropharyngeal edema without abscess formation, and echocardiogram showing mitral insufficiency and pericardial effusion. After the patient was given IVIG with antibiotics were stopped, there was a dramatic improvement in the patient’s symptoms and signs of inflammation.
Traditionally, confirming the presence of an underlying infection rules out KD. All tests performed to determine whether there were other underlying diseases causing the patient’s clinical symptoms revealed negative results. The patient exhibited typical features of KD, abnormal echocardiogram findings, increased platelet counts, and ultimately showed typical thick subungual desquamation of KD. Studies have shown that children with coronary artery lesions on echocardiography are at increased risk of developing pericardial effusion and mitral valve insufficiency when diagnosed with KD [4]. In the current case, the patient was promptly diagnosed with KD and given IVIG within the first ten days of fever onset. This may have helped prevent the development of coronary arterial complications even in patients with an ambiguous clinical course. It has been reported that acute reactants reach peak levels on day 6 after fever onset in patients who typically present with KD [5]. Notably, the patient in this case presented with the symptoms of KD on day 6 when the severity of the suppurative cervical lesion was at its highest and the serum levels of CRP reached their maximum. It is impossible to clearly differentiate between suppurative cervical lymphadenopathy and non-suppurative lymphadenopathy with just an inspection. A CT scan showed lower Hounsfield units for radiolucent foci in the retropharyngeal space, suggesting phlegmon and pre-inflammatory changes. There are several reports of patients with KD who were initially suspected of having a deep neck infection on radiological examinations [6-8].
Recently, there was a report attempting to define the clinical features of KD that initially mimic retropharyngeal abscess [9]. There are few pathological reports on the acute phase of KD due to the relatively smaller number of patients with KD who require lymph node biopsy to establish a diagnosis of KD [10,11]. KD patients generally show focal necrosis accompanied by infiltration of inflammatory cells, such as neutrophils and macrophages in the marginal zone of the cervical lymph nodes during the acute phase of KD [10]. Yokouchi et al. reported that the acute phase of KD is histopathologically characterized by necrotic foci beneath the capsule of lymph nodes, and it is also accompanied by fibrin thrombi in the small vessels and perivascular nuclear debris [11]. In conclusion, although there may be presumptive diagnostic clues to an underlying infection in the acute phase, clinicians should consider KD as a differential diagnosis until KD is completely ruled out.
